
The Cost of Caring in 2025: Why Health Systems Must Take Action Now
Hospitals are navigating a financial crisis in 2025. Soaring labor costs, Medicare and Medicaid underpayments, and complex regulatory demands are pushing U.S. health systems to the brink, as detailed in the American Hospital Association’s 2025 Cost of Caring Report. The solution lies in leveraging CMS-mandated transparency data to empower smarter reimbursement strategies.
At Trek Health, our AI-powered Competitive Market Analysis (CMA) platform transforms healthcare payments by turning over a petabyte of CMS transparency data into actionable insights. We help hospitals close reimbursement gaps, negotiate stronger contracts, and ensure compliance with CMS price transparency rules. Ready to take control? Let’s explore the challenges and solutions.
The Financial Crisis Facing Hospitals
The AHA’s 2025 Hospital Cost Report highlights the mounting pressures threatening hospital sustainability. Here’s what hospitals are up against:
- Surging Labor Costs: Labor accounts for 56% of hospital expenses, with nurse salaries rising 26.6% faster than inflation since 2021.
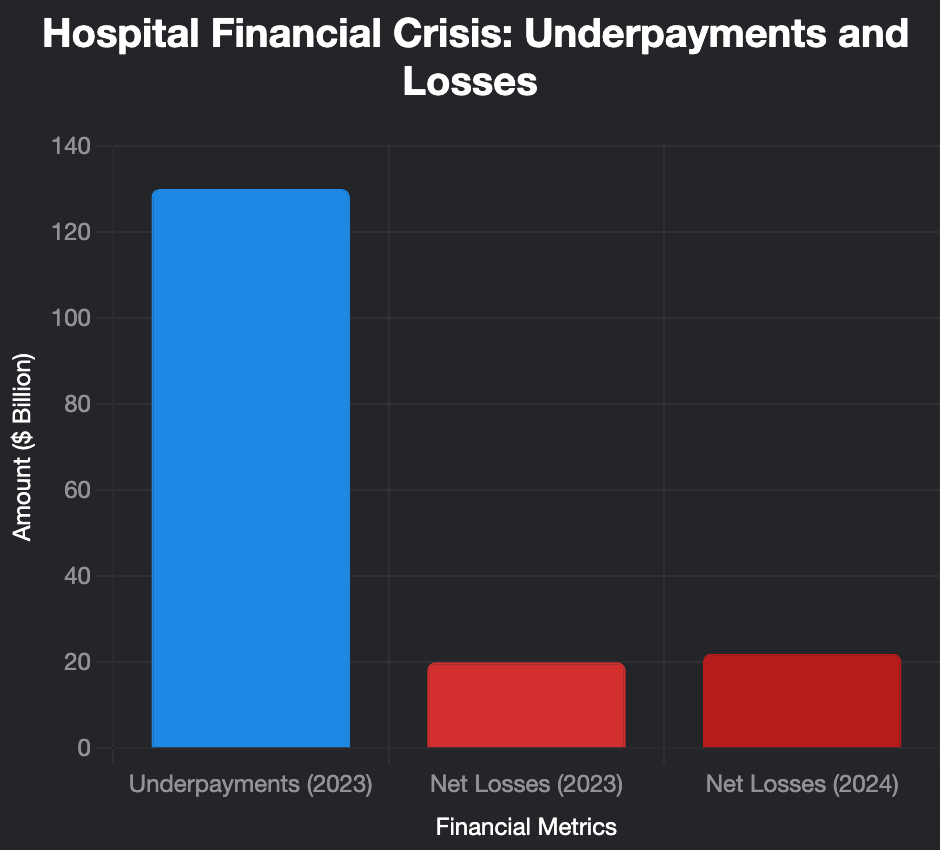
- Massive Underpayment Gaps: In 2023, Medicare and Medicaid underpaid hospitals by $130 billion.
- Rising Utilization: Emergency visits for heart failure surged 126.7% per capita from 2010–2019, with related spending up 177.2%.
- Medicare Advantage (MA) Struggles: In 2024, MA observation stays were 36.9% longer than Traditional Medicare, yet only 49% of costs were reimbursed.
- Administrative Burden: MA plans issued 50 million prior authorizations in 2023, driving $26 billion in claims management costs—a 23% year-over-year increase.
- Supply Chain Vulnerabilities: With 70% of medical devices and 90% of generic injectable drugs sourced internationally, shortages can spike costs by up to 15%.
These pressures threaten patient care and financial viability. Hospitals need data-driven tools to fight back.
How Trek Health’s CMA Platform Helps
Hospitals rely on commercial contracts to offset public payer losses, but outdated tools limit negotiation power. Trek Health’s CMA platform leverages CMS’s machine-readable file (MRF) data to deliver real-time insights, enabling providers to:
- Pinpoint Under-Reimbursed Services: Identify services with reimbursement shortfalls instantly using CMS data analytics.
- Simulate Negotiations: Model rate increases to prepare for payer discussions, maximizing contract value.
- Secure Better Contracts: Achieve rate hikes with major payers.
- Stay CMS-Compliant: Ensure MRFs meet CMS’s updated guidance, avoiding penalties of up to $5,500 per day.
FAQs: Navigating Hospital Financial Pressures in 2025
Why are hospitals under such financial strain?
Rising labor costs, $130 billion in underpayments, and a 23% increase in administrative costs from prior authorizations are key drivers (AHA).
How does Trek Health’s CMA platform help?
It leverages CMS transparency data to identify underpayments, simulate negotiation scenarios, and secure better contracts while ensuring compliance.
What’s the issue with Medicare Advantage?
MA plans have longer stays but reimburse only 49% of costs compared to Traditional Medicare, squeezing margins (AHA).
How can hospitals stay CMS-compliant?
Publish accurate MRFs per CMS guidelines. Trek Health’s platform ensures compliance with current and upcoming requirements.
Take Control of Your Financial Future
With a $130 billion reimbursement gap and increasing regulatory demands, hospitals can’t rely on outdated systems. Trek Health’s AI-powered CMA platform puts CMS transparency data to work, helping you optimize contracts, protect margins, and stay compliant.
Act Now:
- Book a Demo to see the CMA platform in action.
- Explore Careers to join Trek Health’s mission.
- Stay up to date with our resources.
Stay informed, stay compliant, and stay profitable with Trek Health.
Sources:
- American Hospital Association (AHA)
- Kaiser Family Foundation (KFF)
- Centers for Medicare & Medicaid Services (CMS)
- Healthcare Financial Management Association (HFMA)
- Health Affairs
- America’s Health Insurance Plans (AHIP)
.png)
White Paper
From Transparency to Prediction: Quantifying the Drivers of Physician Reimbursement Variation
This analysis uses Transparency in Coverage data to model how payers behave, not just what they pay. By linking reimbursement rates to physician characteristics, we uncover the patterns behind payment variation and transform transparency data into predictive intelligence. The result: a predictive view of rate dynamics that helps stakeholders anticipate trends and negotiate with data-driven confidence.

White Paper
Q1 2026 State of Commercial Reimbursement: Trek Health’s Quarterly Market Intelligence
As Trek Health's Quarterly Market Intelligence series matures, more longitudinal trends are emerging. After a brief period of stabilization in late 2025, Q1 2026 brought renewed payer pressure across specialties, geographies, and major national payers. Trek Health's latest Quarterly Market Intelligence report breaks down exactly what shifted — and what it means for your contracts.
Want to see how these trends affect your market? Speak to our team.

White Paper
Q3 2025 State of Commercial Reimbursement: Trek Health’s Quarterly Market Intelligence
Trek Health’s Quarterly Reimbursement Brief highlights emerging variability in commercial payment rates across U.S. payers, specialties, and geographic markets. With some segments experiencing double-digit growth and others notable declines, contracting performance is increasingly shaped by real-time payer behavior rather than historical norms. Through validated reimbursement trend analytics, contract intelligence, and policy monitoring, Trek equips provider organizations to anticipate market shifts, protect revenue, and negotiate with measurable leverage.

White Paper
Q4 2025 State of Commercial Reimbursement: Trek Health’s Quarterly Market Intelligence
Trek Health’s Q4 2025 Quarterly Market Intelligence report analyzes quarter-over-quarter commercial reimbursement movement across national payers, physician specialties, and U.S. states. While overall reimbursement improved following earlier declines, rate changes remained uneven—highlighting payer selectivity, persistent specialty outliers, and shifting geographic leverage. This report moves beyond static benchmarks by tracking real-time reimbursement changes, giving provider organizations actionable insight to identify negotiation risk early, protect rate parity, and respond proactively to evolving payer behavior.

White Paper
Reimbursement and Reality: The Economics of Breast Cancer Treatment
While breast cancer awareness efforts often focus on screening and treatment, one critical factor remains overlooked: how care is reimbursed. Payment structures shape far more than provider margins; they influence access, equity, and patient outcomes.
In this analysis of payer rates, Trek Health uses its Transparency Platform to analyze how reimbursement for breast cancer care varies across geography, commercial payer behavior, and public policy. The findings reveal a system that rewards disease burden rather than prevention which creates inequities that ripple through the entire care process.
Inside you’ll learn:
- How reimbursement rates differ dramatically by state and payer
- Why higher disease burden correlates with higher payment, but prevention does not
- What these trends mean for provider strategy, patient access, and equity
Download the full analysis to see how transparency data can help reshape breast cancer care—turning financial insight into fairer outcomes.

White Paper
Telehealth Parity: Are You Getting Reimbursed When Doing What’s Right for the Patient?
Telehealth reimbursement fell below in-office rates in 98% of observations across major commercial payers for established patient visits. State parity laws showed no association with improved commercial reimbursement equity, a finding explained in part by ERISA preemption of self-funded employer plans.
Read the full analysis for payer-level breakdowns and implications for federal policy.

White Paper
The Cost of Policy Drift: A Framework for Measuring and Managing Payer Policy Lag as an Operational Risk
Commercial payers change coverage criteria, prior authorization requirements, and coding guidelines continuously and without standardized notice, leaving provider organizations to detect, interpret, and operationalize each update on their own. The lag between when a payer changes a rule and when that change is fully reflected in an organization's workflows is a distinct, measurable operational risk we term Policy Drift. Left unnamed and unmeasured, Policy Drift generates denial volume, prior authorization friction, fee schedule underpayment, and audit exposure that most organizations misattribute to clinical or documentation failure.
This paper introduces a four-stage latency framework for decomposing Policy Drift into its constituent components, a KPI set for tracking it, and the infrastructure requirements for closing it systematically.

White Paper
The Economics of Payer Contract Management Automation: Quantifying Cost Savings & Revenue Lift
Trek Health's Contract Intelligence (CI) automates contract interpretation and policy maintenance, transforming unstructured payer data into actionable rules. Using industry benchmarks and multi-scenario modeling across clinic, multispecialty, and hospital environments, CI generates annual savings ranging from $80K to over $9.3M, driven by avoided denials, reduced administrative labor, and streamlined policy-update workflows. Our results show that CI functions as core financial infrastructure rather than a point solution, delivering structural value across the reimbursement lifecycle.

White Paper
The Payer Paradox: When Higher Rates Don’t Mean Higher Reimbursement
This analysis uncovers a critical paradox in commercial healthcare financing: the payers offering the highest contracted rates often deliver the lowest realized reimbursement once denials and administrative friction are accounted for. By introducing the Payer Generosity Index (PGI) and adjusted PGI (aPGI), Trek Health reveals how payer performance varies not only across insurers, but across specialties and service lines. These findings equip healthcare organizations with a clearer, data-driven framework for contracting, revenue optimization, and strategic planning in an increasingly complex reimbursement landscape.

White Paper
The Private Practice Playbook: Rate Negotiation Index Rankings for Specialty-Specific M&A Strategy
Physician economics are shifting as private equity and independent platforms redefine the workforce landscape. Trek Health’s Rate Negotiation Index Report quantifies the return on physician labor across states and specialties in a new lens: combining commercial reimbursement, physician salary, malpractice risk, and provider density into a single metric. This data driven foundation for smarter M&A strategy identifies the most economically sustainable opportunities across the U.S. for physician recruitment and network expansion.

Hospitals are navigating a financial crisis in 2025. Soaring labor costs, Medicare and Medicaid underpayments, and complex regulatory demands are pushing U.S. health systems to the brink, as detailed in the American Hospital Association’s 2025 Cost of Caring Report. The solution lies in leveraging CMS-mandated transparency data to empower smarter reimbursement strategies.
At Trek Health, our AI-powered Competitive Market Analysis (CMA) platform transforms healthcare payments by turning over a petabyte of CMS transparency data into actionable insights. We help hospitals close reimbursement gaps, negotiate stronger contracts, and ensure compliance with CMS price transparency rules. Ready to take control? Let’s explore the challenges and solutions.
The Financial Crisis Facing Hospitals
The AHA’s 2025 Hospital Cost Report highlights the mounting pressures threatening hospital sustainability. Here’s what hospitals are up against:
- Surging Labor Costs: Labor accounts for 56% of hospital expenses, with nurse salaries rising 26.6% faster than inflation since 2021.
- Massive Underpayment Gaps: In 2023, Medicare and Medicaid underpaid hospitals by $130 billion.
- Rising Utilization: Emergency visits for heart failure surged 126.7% per capita from 2010–2019, with related spending up 177.2%.
- Medicare Advantage (MA) Struggles: In 2024, MA observation stays were 36.9% longer than Traditional Medicare, yet only 49% of costs were reimbursed.
- Administrative Burden: MA plans issued 50 million prior authorizations in 2023, driving $26 billion in claims management costs—a 23% year-over-year increase.
- Supply Chain Vulnerabilities: With 70% of medical devices and 90% of generic injectable drugs sourced internationally, shortages can spike costs by up to 15%.
These pressures threaten patient care and financial viability. Hospitals need data-driven tools to fight back.

How Trek Health’s CMA Platform Helps
Hospitals rely on commercial contracts to offset public payer losses, but outdated tools limit negotiation power. Trek Health’s CMA platform leverages CMS’s machine-readable file (MRF) data to deliver real-time insights, enabling providers to:
- Pinpoint Under-Reimbursed Services: Identify services with reimbursement shortfalls instantly using CMS data analytics.
- Simulate Negotiations: Model rate increases to prepare for payer discussions, maximizing contract value.
- Secure Better Contracts: Achieve rate hikes with major payers.
- Stay CMS-Compliant: Ensure MRFs meet CMS’s updated guidance, avoiding penalties of up to $5,500 per day.
FAQs: Navigating Hospital Financial Pressures in 2025
Why are hospitals under such financial strain?
Rising labor costs, $130 billion in underpayments, and a 23% increase in administrative costs from prior authorizations are key drivers (AHA).
How does Trek Health’s CMA platform help?
It leverages CMS transparency data to identify underpayments, simulate negotiation scenarios, and secure better contracts while ensuring compliance.
What’s the issue with Medicare Advantage?
MA plans have longer stays but reimburse only 49% of costs compared to Traditional Medicare, squeezing margins (AHA).
How can hospitals stay CMS-compliant?
Publish accurate MRFs per CMS guidelines. Trek Health’s platform ensures compliance with current and upcoming requirements.
Take Control of Your Financial Future
With a $130 billion reimbursement gap and increasing regulatory demands, hospitals can’t rely on outdated systems. Trek Health’s AI-powered CMA platform puts CMS transparency data to work, helping you optimize contracts, protect margins, and stay compliant.
Act Now:
- Book a Demo to see the CMA platform in action.
- Explore Careers to join Trek Health’s mission.
- Stay up to date with our resources.
Stay informed, stay compliant, and stay profitable with Trek Health.
Sources:
- American Hospital Association (AHA)
- Kaiser Family Foundation (KFF)
- Centers for Medicare & Medicaid Services (CMS)
- Healthcare Financial Management Association (HFMA)
- Health Affairs
- America’s Health Insurance Plans (AHIP)

